K__ at Feminists with FSD: Notes on MTV’s True Life: I Can’t Have Sex
Actual, proper terminology was used throughout the show. Chronic pelvic pain conditions were named, but some conditions that overlap were not mentioned at all (interstitial cystitis, for example, was not explored in this episode. This is a shame – interstitial cystitis is another misunderstood condition which would benefit from careful media coverage.) This episode focused on the impact of chronic pelvic pain on the women’s sex lives. And that means that while you could learn a little about life with chronic pelvic pain from this episode, for a clinical discussion and details on specific conditions and available treatments, you’ll need to look elsewhere.
Carol at Aspieadvocate: I’m an Embarrassment
Yeah, I know some parents of autistic kids worry about the kids embarrassing the rest of the family in public with their unusual behavior. But for me it’s the other way around. I never shut up about autism, mine or his, and while I have every right to out myself, I’m making decisions about him that should really be his to make. Except even if he’s made different decisions about disclosure than I have, he’s not (yet) verbal enough to tell anyone.
David Gorksi at Science-Based Medicine: Death by “alternative” medicine: Who’s to blame? [trigger warning]
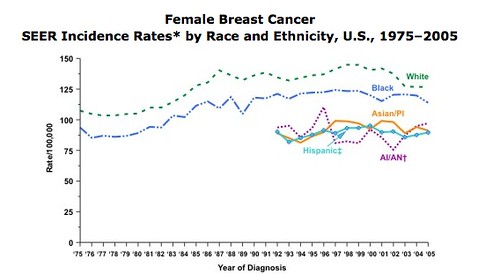
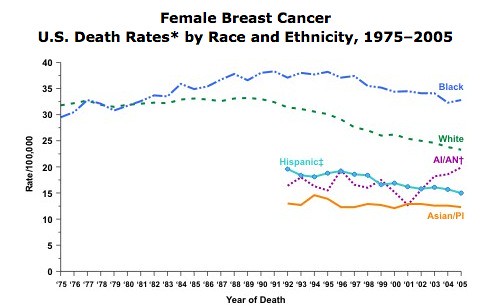
Of course, the implication of “Secret” thinking is that, if you don’t get what you want, it’s your fault, an idea that also resonates with so much “alternative” medicine, where a frequent excuse for failure is that the patient either didn’t follow the regimen closely enough or didn’t want it badly enough. Basically, The Secret is what inspired Kim Tinkham to eschew all conventional therapy for her breast cancer and pursue “alternative” therapies, which is what she has done since 2007. Before I discuss her case in more detail, I’m going to cut to the chase, though.
This weekend, I learned that Kim Tinkham’s cancer has recurred and that she is dying.
Arwyn at Raising My Boychick: How far I’ve come
Eight years ago I was withdrawing from college. Again. I’d started medication, divalproex sodium, and that was going to cure me; we’d packed up our possessions, bought furniture in flat boxes, and drove it most of the way across the country to this town with one redeeming feature: the college from which I had just withdrawn because it was better than flunking out from chronic absences. I did not know who I was, what good I was, if I could not do college, be a student. I could not see a future, and mostly did not believe I had one.
Linsay at Autist’s Corner: Autism-related gene spotlight: CNTNAP2
EXECUTIVE SUMMARY: CNTNAP2 is a large gene near the end of chromosome 7 that encodes a cell-adhesion protein involved in distributing ion channels along axons (the long tails of nerve cells) and in attaching the fatty cells making up the myelin sheath to the surface of the axon. DIsruptions in this gene have been associated with autism, epilepsy, Tourette syndrome and other neurodevelopmental disorders. Variations at certain points within the gene that don’t alter or disrupt its expression have also been associated with an increased likelihood of autism.